- Due to covid-19 only online consultation is available. Write at this email to consult your trusted doctor, Dr. Sharmila Majumdar
- mili77@gmail.com
Fertility and Infertility

Zinc and its importance in Male Fertility
December 28, 2017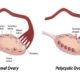
Everything you need to know about Polycystic Ovarian Disease (PCOD)
January 4, 2018Fertility is the ability to conceive and have children. Most of us take our fertility for granted but the process of reproduction is complex and sometimes couples experience difficulties when they try to have a baby. If you are planning to have a baby there are some things you and your partner can do to improve your chance of conceiving and having a healthy baby. Infertility is defined as the inability to conceive after 12 months or more of unprotected intercourse.
About one in nine couples experience fertility difficulties. There are many reasons for this, some relating to the male partner and some to the female partner. If you suspect an infertility problem , talk to your Sexologist, infertility specialist who will guide you through the steps of an infertility investigation.
For people who have been diagnosed with cancer, fertility preservation is an important consideration if there is a chance that their cancer treatment may affect their fertility. Increasingly, fertility preservation is now also being used for non-medical purposes. Egg freezing for social reasons has seen a rise in demand in recent years.
Suspecting infertility
Most people take their fertility for granted and do not expect to have problems conceiving. However, one in nine couples experience fertility difficulties.
What to do if you suspect a problem
If you have been trying to conceive for a year or more, it is time to seek medical advice. If you are over 35, you should see a doctor if you have been trying to conceive for six months or more.
The first point of contact should be your general practitioner (GP) who will start an infertility investigation. This involves a detailed medical history and a physical examination of both partners and some basic tests to make sure that the woman is ovulating and that the man produces sperm. If everything seems in order, your GP may advise you to keep trying for a little longer before consulting a fertility specialist. However, if your test results indicate a problem, your doctor will refer you to a fertility specialist without delay. The fertility specialist will do more tests to establish the cause of infertility and determine the type of treatment you may need.
Causes of infertility
There are many reasons why pregnancy does not occur. About one-third of infertility cases are due to male factors and one-third due to female factors. Sometimes both partners have a fertility problem. In about 20 per cent of cases, there is no apparent cause of infertility, so-called unexplained or idiopathic infertility. As more couples delay childbearing age-related infertility is becoming more common.
Dealing with infertility
A diagnosis of infertility often comes as a shock. It is unexpected and unwelcome and emotionally challenging. Unlike other adverse life events, which may have a clear resolution, infertility is uniquely distressing because it can last for many years and the outcome is uncertain. Some people find it helpful to discuss their feelings with a psychologist or counsellor. Others feel better if they take action by starting treatment.
What to do next
Once the cause of infertility has been pin-pointed, your doctor will discuss treatment options with you. These will vary depending on the cause of infertility but will most likely involve some form of assisted reproductive treatment. You need a referral from your GP to see a fertility specialist. Your GP may recommend a fertility specialist, unless you have a preference for a particular ART clinics or individual fertility specialist.
The chance of ART treatment working has greatly improved since the late seventies when the first IVF baby was born. Although your chance of having a baby with ART depends largely on factors that are beyond your control, there are some things that you can do to improve the odds. The lifestyle factors that influence the chance of natural conception for both men and women also affect your chance of ART success.
Understanding reproduction
It is useful to understand how eggs and sperm are normally formed, and how conception occurs to understand the causes of infertility and how they are targeted in ART.
The hormones which control the production of sperm and eggs are called gonadotropins. There are two types of gonadotropins: follicle-stimulating hormone (FSA) and luteinising hormone (LH). In men, they stimulate the testicles to produce sperm and testosterone. In women, they act on the ovaries, where the eggs develop. The female sex hormones, oestrogen and progesterone, are produced by the ovaries when eggs mature and are released (ovulation).
The production of sex hormones and the release of an egg is known as the menstrual cycle. It is counted from the first day of the period until the day before the start of the next period. In an average cycle of 28 days, ovulation happens on day 14. However, and it is important to note that, ovulation occurs earlier in women with shorter cycles and later in women with longer cycles.
Your fertility and timing
Sperm are produced at the rate of about 300 million per day. They take some 80 days to mature. Each sperm has a head, which contains the genetic material, and a tail, which propels it up through the vagina, uterus, and Fallopian tubes where the conception occurs when an egg and a sperm come together. At ovulation, an egg is released from the ovary into the fallopian tube. If sperm is present at that time, the egg can be fertilised. The fertilised egg then starts to divide and becomes an embryo. After ovulation, the ovary produces progesterone which prepares the lining of the uterus – the endometrium – for the growing embryo. If an embryo does not form or attach to the endometrium (implantation), the level of progesterone drops and the next period starts.
A few days after implantation, the embryo starts to produce Human Chorionic Gonadotropins (HCG) – the hormone that gives a positive pregnancy test reading.
Dr. Sharmila Majumdar
Chief Consultant Sexologist
Sexual and Mental Health Clinic
Avis Hospital, Jubilee hills
Next to Chiranjivee Blood Bank
Hyderabad 500033

1 Comment
A great post. Thanks doctor